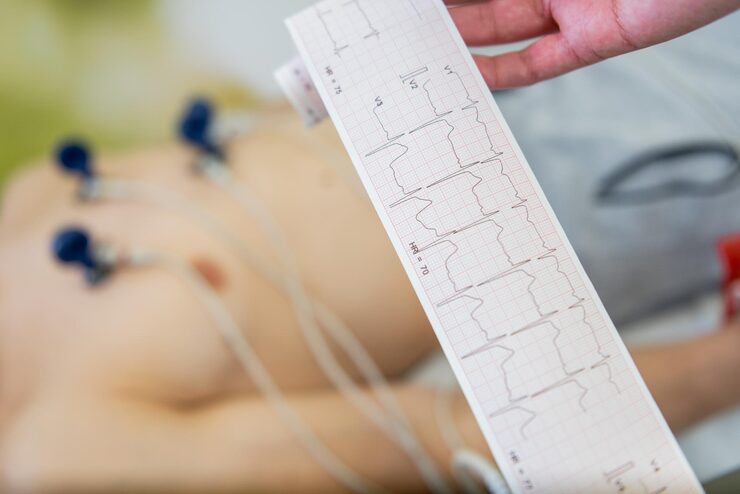
Electrocardiography (ECG) remains a cornerstone of cardiovascular care, with the 12-lead ECG recognized as the diagnostic gold standard for comprehensive heart evaluation. It provides a multi-angle view of cardiac electrical activity, enabling clinicians to detect a wide range of conditions, including ischemia, structural abnormalities, and conduction disorders.
In contrast, single-lead ECG focuses on heart rhythm monitoring, making it highly effective for detecting arrhythmias and supporting continuous tracking outside clinical settings . Unlike the clinically administered 12-lead ECG, single-lead devices are compact, wearable, and designed for everyday use. Solutions such as FibriArt� extend monitoring into real-world environments, complementing clinical diagnostics with accessible, real-time heart rhythm insights.
Clinical Perspective: What Each ECG Modality Offers
A 12-lead ECG provides a comprehensive, multi-vector assessment of cardiac electrical activity. This enables clinicians to identify ischemia, evaluate cardiac axis, detect chamber enlargement, and diagnose complex conduction abnormalities with high precision.
A single-lead ECG records electrical activity along a single vector. While this limits spatial analysis, it retains clear visibility of P, QRS, and T waveforms, making it suitable for rhythm interpretation and interval measurement in ambulatory settings.
This fundamental difference defines their clinical use:
- 12-lead ECG for detailed diagnosis
- Single-lead ECG for monitoring and screening
Arrhythmia Detection: Where Single-Lead ECG Excels
Single-lead ECG devices have demonstrated strong clinical performance in detecting arrhythmias, especially atrial fibrillation (AF), which is one of the most common and clinically significant rhythm disorders.
Studies consistently show:
- High sensitivity and specificity for AF detection
- Reliable identification of irregular heart rhythms
- Effective capture of intermittent or symptom-triggered events
In addition to AF, single-lead ECG can detect:
- Premature atrial contractions (PACs)
- Premature ventricular contractions (PVCs)
- Basic tachyarrhythmias
However, more complex arrhythmias and detailed conduction abnormalities may still require multi-lead ECG evaluation for confirmation.
Looking for detailed clinical validation?
Explore in-depth research and comparative analysis on ECG technologies.
Read our White Paper: Single-Lead vs 12-Lead ECGPQRST Interval Measurement: What Single-Lead Can Deliver
Beyond rhythm detection, single-lead ECG devices are capable of measuring important cardiac intervals.
They provide:
- Accurate heart rate and RR interval measurements
- Clinically useful estimates of PR, QRS, and QT/QTc intervals
The accuracy of these measurements depends on signal quality, device calibration, and user conditions. Factors such as motion artifacts or poor electrode contact can affect waveform clarity.
For critical clinical decisions especially those involving QT interval abnormalities-confirmation using a 12-lead ECG is recommended.
Why Wearable ECG Devices Are Transforming Cardiac Monitoring
The increasing adoption of wearable ECG technology reflects a shift toward more proactive and accessible healthcare.
Continuous Monitoring in Real Life
Unlike traditional ECG tests, wearable devices enable long-term monitoring, improving the chances of detecting intermittent or asymptomatic arrhythmias.
Accessibility and Convenience
Single-lead devices are compact and easy to use, allowing individuals to monitor their heart during daily activities-whether at work, at the gym, or at home.
Real-Time Data and Remote Care
Wireless connectivity allows ECG data to be shared instantly with healthcare providers, supporting faster decision-making and telemedicine workflows.
Improved Patient Engagement
Wearable devices empower users to take a more active role in managing their heart health.
Limitations That Define Its Role
While single-lead ECG offers clear advantages, it also has important limitations:
- It cannot provide full spatial analysis of the heart
- It is not suitable for diagnosing ischemia or structural abnormalities
- Signal quality may be affected by movement or external interference
- False positives may occur in certain rhythm interpretations
These limitations highlight that single-lead ECG is best used as a monitoring and screening tool, rather than a replacement for diagnostic ECG.
When to Use Single-Lead vs 12-Lead ECG
Single-lead ECG is ideal for:
- Detecting and monitoring arrhythmias
- Recording symptoms such as palpitations
- Long-term cardiac tracking
- Remote patient monitoring
12-lead ECG is essential for:
- Diagnosing heart attacks and ischemia
- Comprehensive cardiac evaluation
- Detailed conduction and structural analysis
Together, they form a complementary approach to cardiac care.
FibriArt� in the Evolving Landscape of Cardiac Monitoring
As cardiac care increasingly shifts beyond traditional clinical settings, the role of wearable ECG technologies has become more prominent. Solutions such as FibriArt� are aligned with this transition, supporting a model of care that extends monitoring into everyday environments while maintaining clinical relevance.
Rather than serving as a replacement for conventional diagnostic tools, FibriArt fits within a complementary framework-enabling consistent rhythm tracking outside the clinic and providing data that can support timely clinical evaluation when needed. This approach helps bridge the gap between episodic testing and continuous monitoring.
By contributing to more accessible and ongoing cardiac assessment, FibriArt reflects the broader evolution of healthcare toward preventive, data-driven, and patient-centric monitoring.
Explore the Complete Research
If you are evaluating ECG technologies or want a deeper understanding of single-lead vs 12-lead performance, our white paper provides a detailed, evidence-based analysis.
Read Our White PaperConclusion
Single-lead ECG technology has become an important component of modern cardiac care, particularly for arrhythmia detection and continuous monitoring. While the 12-lead ECG remains essential for comprehensive diagnosis, wearable single-lead devices offer a practical solution for real-world heart monitoring.
By combining both approaches, healthcare providers and individuals can benefit from improved accessibility, earlier detection, and more informed decision-making-ultimately supporting better cardiovascular outcomes
FAQ
The main difference is the breadth of information. A single-lead ECG provides one view of the heart's rhythm, while a 12-lead ECG provides twelve different electrical perspectives, allowing doctors to see the heart's three-dimensional activity.
No. A single-lead ECG is designed to detect heart rate and rhythm irregularities. It lacks the multiple viewpoints required to identify the specific signs of muscle damage or blood flow blockage associated with a heart attack.
They are popular because of convenience and early detection. They allow users to capture "as-it-happens" data during symptoms that might not occur during a doctor's visit, making them excellent for catching intermittent issues like AFib.
No. It is a screening tool, not a diagnostic one. While it can flag an abnormality, a 12-lead ECG is almost always required to confirm a diagnosis and determine the underlying cause.
Both play a role. A single-lead ECG is better for daily monitoring and tracking trends over time, whereas a 12-lead ECG is the gold standard for clinical evaluation and emergency diagnostics.